TMJ Symptoms
Chronic jaw, face and neck pain
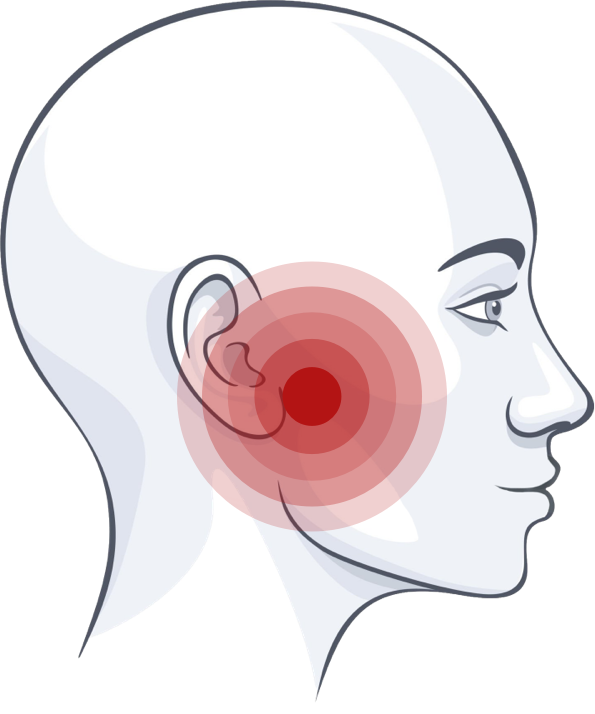

Understanding Jaw Pain
When jaw, face, or neck pain becomes ongoing
Jaw, neck, and facial pain can begin gradually or appear after a specific event such as injury, dental treatment, or prolonged stress. For some people the discomfort settles within a short period. For others the symptoms persist or return over time, sometimes becoming part of daily life.
Patients often describe feeling unsure about where the pain is coming from, particularly when the discomfort moves between the jaw, face, temples, or neck. This pattern is not unusual.
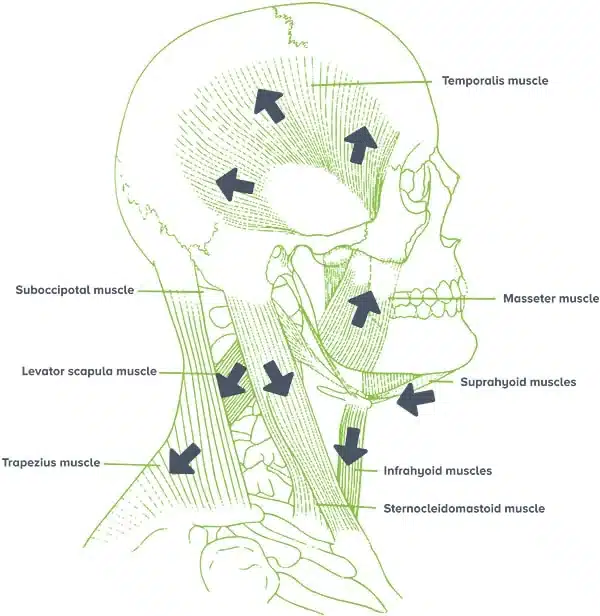
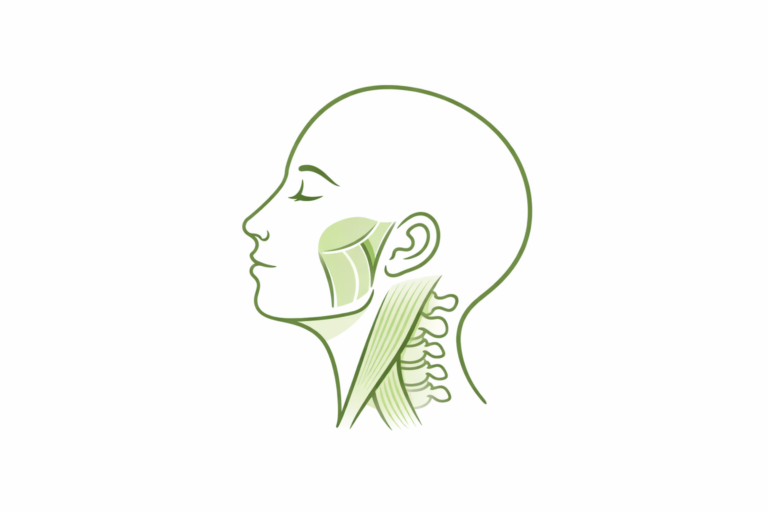
The jaw joints and surrounding muscles are closely connected with structures in the head and neck. Because of this, symptoms in one area are often felt in others.
Areas where pain may be felt
- Around the jaw joints
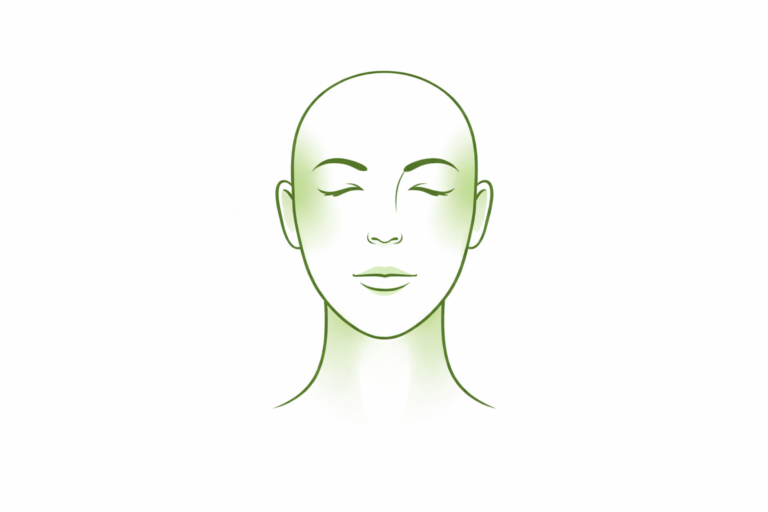
- In the cheeks or temples
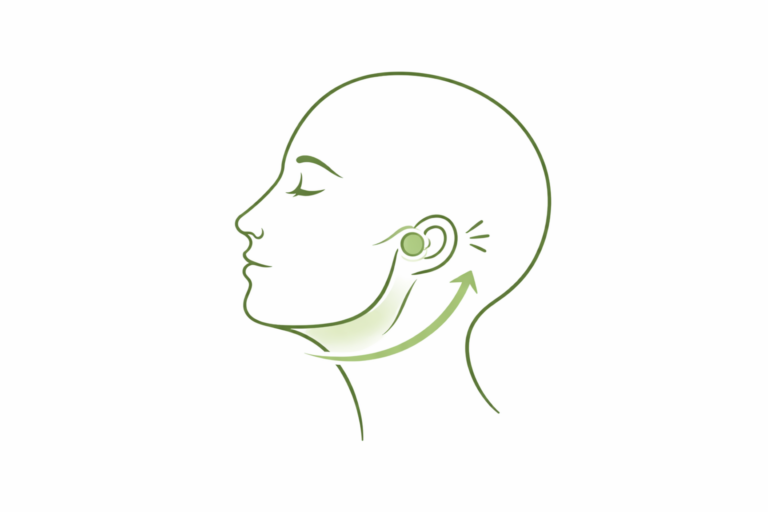
- In front of the ears
- Along the sides of the face
- In the neck or base of the skull
Pain may remain in one area or shift between these locations.
Recognising Symptoms
Jaw pain can feel different for everyone
People describe chronic jaw or facial pain in different ways. For some it feels like a persistent ache. For others the discomfort appears as sharp pain, pressure, or muscle fatigue.
Patients commonly describe
- Persistent aching or soreness
- Sharp or stabbing pain
- Pressure around the temples or jaw joints
- Tight or burning sensations in the jaw muscles
- Fatigue when talking or chewing
Some people notice symptoms mainly when using the jaw. Others experience discomfort even when the jaw is resting. The location of pain does not always reflect where the underlying strain or irritation is occurring.

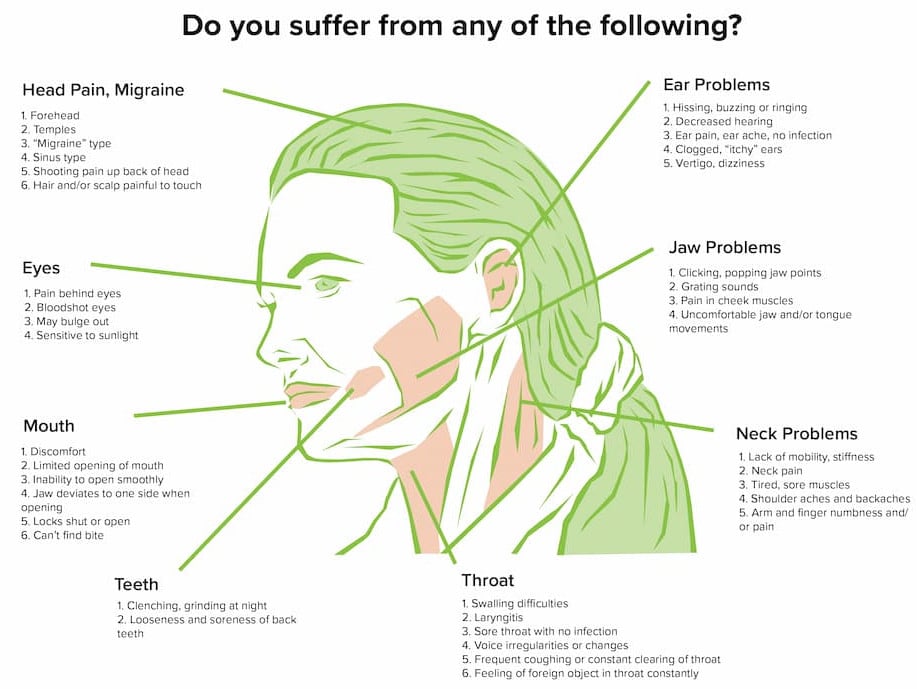
Connected Symptoms
Jaw pain often appears with other symptoms
Many people experiencing chronic jaw or facial pain notice other symptoms developing at the same time. Because the jaw joints, muscles, and nerves work as a connected system, changes in one area can influence nearby structures.
Symptoms that may occur alongside jaw pain
- Jaw clicking or popping
- Stiffness when opening the mouth
- Headaches or pressure in the temples
- Neck tension or discomfort
- Ear fullness or ear pain
- Facial muscle fatigue
- Teeth clenching or grinding
Sometimes these symptoms appear together. At other times they occur separately or change over time. Understanding how these symptoms relate to jaw function often requires careful assessment.
Experiencing more than one symptom?
Many people experiencing jaw pain also notice changes in jaw movement, headaches, or muscle tension. Exploring the full pattern of symptoms can help provide useful context.


Symptom Patterns
Symptoms can change from day to day
Jaw-related symptoms rarely remain exactly the same. Many patients describe periods where symptoms improve, followed by times when discomfort becomes more noticeable again. This fluctuation can feel frustrating, particularly when symptoms seem to return without a clear reason.
Changes in symptoms are often influenced by everyday factors such as:
- stress or fatigue
- prolonged talking or jaw use
- chewing tougher foods
- sleep quality
- physical tension in the head and neck
Fluctuating symptoms are common and do not necessarily indicate that the condition is worsening.
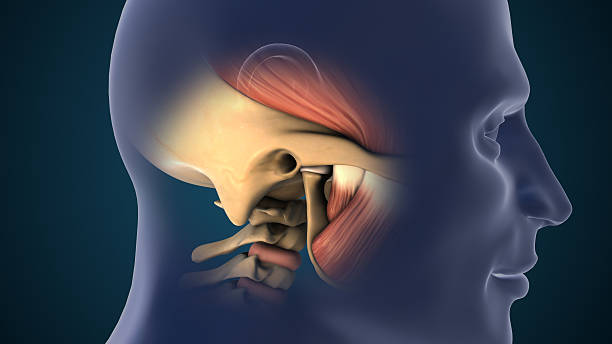
Clinical Insight
A symptom does not always explain the cause
How We Assess
Looking at the whole jaw system
Assessment focuses on understanding how the jaw system is functioning and what factors may be influencing symptoms. The goal is not simply to label a symptom, but to identify patterns that may be affecting the joints, muscles, and surrounding structures.
A clinical evaluation may include:
- discussion of symptoms and medical history
- evaluation of jaw movement and opening patterns
- examination of jaw muscles and joints
- analysis of bite and loading patterns
- imaging where appropriate
This process helps build a clearer picture of how the jaw system is functioning.
Care Planning
Treatment focuses on the underlying drivers
Management of jaw-related symptoms is based on the findings of assessment rather than the symptom name alone. Care plans are personalised and often involve more than one approach.
Care approaches may involve
- orthotic or splint therapy
- strategies to support muscle and joint function
- bite and loading adjustments
- guidance on jaw loading and habits
- collaboration with other health professionals
Care plans are typically staged and reviewed over time as symptoms and jaw function change.

Treatment Options
Learn about TMJ treatment approaches
Our approach to TMJ care
Whole-body care guided by diagnosis
TMJ symptoms rarely come from the jaw alone. They can involve joint mechanics, muscle tension, bite function, posture, breathing, and sleep. At TMJ Centre Melbourne, care begins with understanding why symptoms are occurring. Treatment decisions follow diagnosis, not symptom labels. Care plans are personalised and often combine approaches, with progress reviewed and adjusted over time.
Diagnosis first
Whole-body assessment
Multidisciplinary care
Staged treatment
Considering assessment for ongoing jaw pain?
Persistent jaw, facial, or neck pain can sometimes reflect underlying strain affecting the jaw system. A detailed evaluation can help clarify what may be contributing and what options for management may be appropriate.
When to Seek Advice
When assessment may be helpful
It may be helpful to seek assessment if symptoms:
- persist for several weeks
- return frequently
- interfere with eating or speaking
- occur alongside headaches or neck pain
- involve jaw locking or restricted opening
For many patients, understanding what may be contributing to symptoms provides useful clarity and direction.
Related Symptoms
Explore other TMJ symptoms